Alzheimer’s disease currently affects an estimated one in nine people over the age of 65, a number that shoots up to one in three at 85 (1). Despite its prevalence, there is currently no method for early detection. Now, a team of researchers and engineers at Northwestern University, Illinois, USA, have developed a non-invasive magnetic resonance imaging (MRI) approach to detect Alzheimer’s before patients become symptomatic (2). “We have a new brain imaging method that can detect the toxin that leads to Alzheimer’s disease,” said William Klein, co-leader of the research team and the original discoverer of the amyloid beta protein that causes Alzheimer’s symptoms in the brain. “Using MRI, we can see the toxins attached to neurons in the brain.”
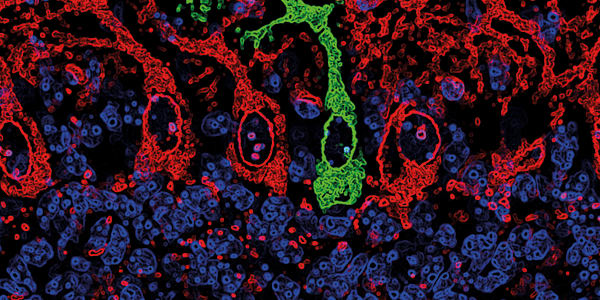
The group’s technology features an MRI probe that couples a magnetic nanostructure with an antibody against amyloid beta proteins, which then show up as dark areas in MRI scans of the brain (see Figure 1). Tested intranasally on mouse models with and without Alzheimer’s disease (as well as on preserved human brain tissue), the scans showed clear differentiation between control and affected brains.

Conventional technologies used to observe Alzheimer’s disease pathology, such as positron emission tomography, detect plaques – abnormal clusters of protein fragments – that only occur in the latter stages of the disease. The new approach detects the amyloid beta oligomers themselves, which can appear as long as a decade before plaques begin to form. Oligomers attack the synapses of neurons, damaging them and ultimately causing neuron death. As time progresses, the oligomers accumulate, forming the amyloid plaques that current probes target. Vinayak Dravid, research team co-leader and Abraham Harris Professor of Materials Science and Engineering, says, “Noninvasive imaging by MRI of amyloid beta oligomers is a giant step forward towards diagnosis of this debilitating disease in its earliest form.”
The new probe isn’t just useful for disease detection – it also conclusively establishes the molecular basis for Alzheimer’s disease. There are currently no effective drugs for the disease, but now that a biomarker has been identified, it may allow researchers to design better treatments. Furthermore, Dravid suggests that the new MRI method could also be used to assess how well a new drug is working: “If a drug is effective, you would expect the amyloid beta signal to go down.” But that’s not all. Preliminary evidence suggests that the MRI probe may also have a therapeutic effect because it directly binds to amyloid beta proteins in the brain. The research team observed that the behavior of mice with Alzheimer’s disease improved even after receiving a single dose of the probe. If the new technology offers both early detection and potential treatment, then it could be the ultimate triumph.
References
- Alzheimer’s Association, “2014 Alzheimer’s disease facts and figures”, Alzheimers Dement, 10, e47– e92 (2014). PMID: 24818261. KL Viola et al., “Towards non-invasive diagnostic imaging of early-stage Alzheimer’s disease”, Nat Nanotechnol, 10, 91–98 (2015). PMID: 25531084.