A Guide to IHC
How immunohistochemical analysis can help navigate the complexities of breast pathology
At a Glance
- Our increasing knowledge of the diverse nature of breast cancer is giving rise to ever more diverse tests
- While molecular tests are increasing in importance, immunohistochemistry (IHC) analysis is just as useful in the differential diagnosis of breast lesions as well as for prognosis and prediction
- IHC can also be used as a tool in the discovery of new therapeutic targets, and in combination as a surrogate for molecular classifications and multigene prognostic panels
- Here, I provide a guide to how IHC analysis can help pathologists make a correct diagnosis and provide accurate prognostic and predictive information to clinicians, and to inform of the factors that might impact IHC test quality
The more we learn about breast cancer, the more we realize just what a broad classification it truly is. Despite what many patients still believe, there’s no one “breast cancer” to rule them all – it’s a heterogeneous group of tumors, and each type exhibits different characteristics, different behaviors and different clinical outcomes. As a result, we’re parlaying this increase in understanding into ever more diverse tests to gain insight into the nature of each individual patient’s disease – and although genomics is an up-and-coming field of study, the molecular tests aren’t the only ones that play a role in tumor classification (1). Immunohistochemistry (IHC) plays an important part too.
Traditionally, IHC analysis has been used for diagnosis in difficult cases, but more recently it has served as a prognostic or predictive marker, as a tool in the search for new therapeutic targets, and even in combination as a surrogate for molecular classifications and multigene prognostic panels. But with a wide range of biomarkers available for IHC testing, it’s important for pathologists to understand what’s out there, how it can be used, and where things might go wrong.
Invasive or in situ?
Myoepithelial (MEP) markers are vital for distinguishing between in situ and invasive tumors; they are present in in situ lesions and absent from invasive lesions (2). Basal-type cytokeratin, smooth muscle myosin heavy chain (SMMHC), smooth muscle actin (SMA), calponin and p63 are frequently used MEP markers – but because they have varying specificity, they’re often used in combination, or alongside the less common collagen IV and laminin markers. For microinvasive carcinoma (≤1 mm), adding keratin staining can highlight the presence of malignant cells.
However, not every invasive tumor follows the rules for MEP markers. Some invasive lesions, like adenoid cystic carcinoma and metaplastic carcinoma, consist of cells that are positive for MEP markers. These cases present a tricky diagnostic challenge, so it’s critical to carefully evaluate the location of MEP marker-positive cells for a correct diagnosis. Also, there’s one benign lesion with unusual MEP marker status: microglandular adenosis, a benign breast lesion that also lacks marker-positive cells (such as p63) and mimics the more aggressive tubular carcinoma. To distinguish the two, check for ER, PR, and S100 status; you’ll find that the benign lesion is negative for the former two and positive for the latter, whereas the carcinoma is the opposite.
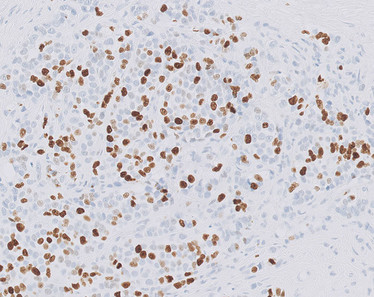
Lobular breast carcinoma (FFPE) stained with anti-Ki-67 antigen.
Pondering papillary lesions
Papillary lesions are a broad group that includes benign, atypical, in situ and even invasive tumors. Because of their diversity, they’re one of the most problematic areas in diagnostic breast pathology – so we routinely use IHC analysis to assist with diagnosis (3). The two most commonly used markers are CK5 for the presence of usual ductal hyperplasia (UDH) and p63 for the presence of MEP cells. What can we diagnose with those two biomarkers?
- Intraductal papilloma (IP): a benign papillary lesion characterized by fibrovascular cores lined with MEP and epithelial layers. IHC analysis for MEP markers highlights the presence of MEP cells along the fibrovascular cores and at the periphery of the lesions.
- IP with UDH or atypical ductal hyperplasia (ADH)/ductal carcinoma in situ (DCIS): the presence of CK5-positive cells can be helpful for diagnosis of florid UDH within an IP; the lack of those cells, along with uniform ER expression, is helpful for diagnosis of IP with ADH/DCIS.
- Intraductal papillary carcinoma (IPC): consists of slender fibrovascular cores covered by a single layer of monotonous neoplastic cells; MEP cells are retained only at the periphery of the lesion.
- Encapsulated papillary carcinoma: a variant of IPC, characterized by fine fibrovascular cores covered by low to intermediate nuclear grade neoplastic cells and surrounded by a fibrous capsule. It lacks MEP cells both at the periphery of the lesion and within the fibrovascular cores and is staged as in situ.
- Solid papillary carcinoma: another variant of IPC that shows a solid growth pattern and inconspicuous fibrovascular cores; it is strongly ER/PR-positive. About two-thirds of these lesions express one or more neuroendocrine markers (4). Smooth nodular borders stage this tumor as in situ regardless of the presence or absence of MEP markers.
Perhaps a better question is: what can’t we diagnose with CK5 and p63? That list is much shorter – only two types of tumor. One is IP with diffuse florid UDH and sclerosis, which can be difficult to differentiate from invasive carcinoma. Benign cytology, strong CK5 positivity, and ER negativity are helpful diagnostic clues. The other exception to the rule is adenomyoepithelial lesion with predominant papillary patterns. This lesion closely resembles IP with MEP hyperplasia, but IHC analysis can highlight its dual ER/PR/HER2-negative epithelial and MEP marker-positive cell populations.
Intraductal hyperplasia: UDH or ADH?
The two intraductal epithelial proliferations – UDH and ADH/low-grade DCIS – are not only biologically distinct, but have very different clinical implications. UDH consists of a heterogeneous proliferation of mixed cells (including luminal, MEP, and even apocrine metaplastic cells), and carries minimal subsequent risk of cancer development (5). A significantly higher risk (three to five times that of the general population) comes from ADH/LG-DCIS, a low-grade monotonous population of luminal cells (6) . To distinguish between the two, pathologists often call on IHC analysis – especially in difficult cases involving necrosis or mitosis, where differential cytokeratin staining can be the key to diagnosis.
What do they look like under a microscope? UDH tends to show a mixed phenotype for low (luminal, such as CK7, CK8, or CK18) and high (basal, such as CK5, CK14, or CK17) molecular weight keratins, along with a heterogeneous or mosaic staining pattern for ER. ADH/LG-DCIS, on the other hand, typically shows restricted luminal cytokeratin expression along with high levels of ER expression. The one exception to this rule is basal-like DCIS, which can sometimes mimic the appearance of UDH. So how can you spot the difference? Neoplastic cells in the more aggressive tumor are usually high nuclear grade, with abundant mitoses and necrosis, and can be negative for ER and PR.
Markers for mysteries
We often use IHC markers to answer specific questions about breast tumors. They can be used to identify lobular lesions, spindle cell involvement, and even trace the origins of metastatic tumors with unknown primaries. These are often clinically important questions – lobular lesions, for instance, behave differently to ductal carcinomas, so it’s impossible to provide a prognosis or select a treatment plan without identifying which of the two you’re facing.
Fortunately, lobular lesions are easily defined by examining two markers: E-cadherin and P120 catenin. Loss of E-cadherin expression is the most consistent molecular change in lobular lesions. IHC analysis of this particular marker is especially helpful when distinguishing between two variants of lobular carcinoma in situ (LCIS): pleomorphic lobular carcinoma in situ (7) and solid LCIS with central necrosis (8). P120 catenin is particularly helpful for clarifying invasive lobular carcinoma lesions with sparse single tumor cells (9), as it demonstrates diffuse cytoplasmic staining, while E-cadherin will only give a negative stain.
The diagnosis of spindle cell lesions, in particular the common metaplastic carcinomas (MC) and phyllodes tumors (PT), often relies on IHC analysis with a panel of IHC markers because the spindle cell component can be deceptively benign or overtly malignant in appearance. Distinguishing between the spindle cells in these two lesions requires a wide spectrum of cytokeratin markers and p63 for MC, as it’s present in over 90 percent of these tumors (10), as well as CD34 for PT, although the amount of staining is inversely associated with PT grade. To confirm or reinforce a diagnosis, look for a biphasic fibroepithelial component (for PT) and the presence of invasive carcinoma of no specific type (for MC), as this is also very helpful.
Comparing the morphology of a metastatic tumor with the original lesion is the single most important step in determining the primary lesion’s origin – but when the primary lesion isn’t available, IHC analysis with markers known with breast specialty can help (see Table 1).
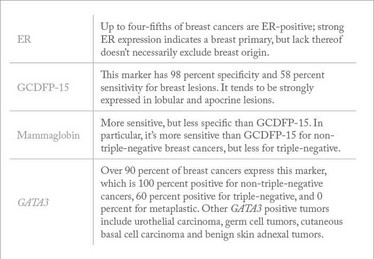
Table 1. Markers with known breast tumor specialty that can assist in identifying a lesion’s origin.
Prognosis and prediction
The use of IHC analyses as predictive tests is fundamentally different from diagnostic classification, because clinicians will use the results from these test directly to guide their management decision; this means that quality specifications and standards are more important than ever. Prognosis and prediction can be conducted using single biomarkers (like ER, PR or HER2) or combinations. Each approach carries its own benefits – and corresponding challenges.
ER and PR, for instance, are expressed in about 75–80 percent and 65 percent of all breast tumors, respectively. ER drives disease progression for positive tumors (those with over 1 percent of tumor cells showing nuclear staining of any intensity), leading to a direct correlation between the level of ER expression and the likelihood of response to hormonal therapies (11). The loss of PR, a transcription factor largely regulated by ER, in ER-positive tumors is associated with decreased response to tamoxifen therapy and a worse overall prognosis (12). Up to one-fifth of invasive breast cancers are also HER2-positive, a trait associated with an aggressive clinical course and poor outcome. But ER, PR and HER2 testing by IHC shouldn’t occur in a vacuum – with an eye to quality, the evaluation should always include normal breast tissue as an internal positive control, and take into account clinical and morphologic features as well.
Hormones aren’t the only biomarkers that can be used for prognosis. Ki-67 is a proliferation marker associated with both poor prognosis and better response to chemotherapy. It can be used to classify breast carcinoma, separating luminal A and B subtypes, and has been included in a number of multiple-gene assays that evaluate the potential for recurrence (13), (14). Why isn’t it more commonly used in the clinic? At the moment, we lack standardized methods for its evaluation, so it hasn’t been recommended for routine breast
cancer evaluation.
Instead, pathologists can consider the wider environment in which the cancer exists – for instance, the context of the patient’s immune system. The tumor microenvironment plays a critical role in the immune-editing process (elimination, equilibrium, and escape). Stromal tumor-infiltrating lymphocytes (sTIL) are a reflex of that environment and can be a powerful prognostic and predictive marker for breast cancer patients, especially in HER2-positive or triple-negative tumors. sTIL should be viewed as a continuous variable; for every 10 percent sTIL increase, there’s a significant reduction in disease-free and overall survival (15). Other immune markers include the current “hot topic,” PD1/PD-L1. Binding between PD1 (expressed on activated T cells) and PD-L1 (expressed on antigen-presenting and tumor cells) results in immune suppression and tumor progression, and the proteins’ upregulation has been associated with poor prognosis in some cancers. Targeted monoclonal antibodies, recently developed, have shown promising and durable responses in many human malignancies – including in a few Phase I studies on breast cancer, with positive response rates between 12–42 percent (16).
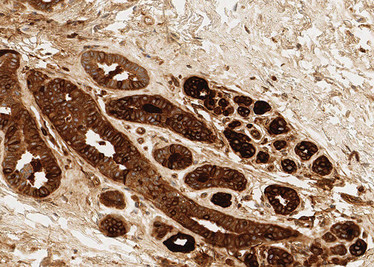
Breast hyperplasia (FFPE) stained with anti-GCDFP-15.
Making use of multiples
Although we’ve used individual breast cancer molecular markers for many years, the concept of using several together was raised after the introduction of molecular classification by gene expression profiling. Many large studies on molecular classification have been performed with IHC surrogates – most commonly ER, PR, and HER2, dividing breast tumors into luminal, HER2-positive and triple-negative. Adding Ki-67 separates luminal A and B subtypes, whereas adding CK5 and epidermal growth factor receptor (EGFR) separates basal-like from non-classified triple-negative breast cancer. More recently, biomarkers such as androgen receptor and p53 have been shown to further stratify these molecular subtypes (17).
The IHC4 score is an assay developed using a retrospective cohort of 1,125 ER-positive breast cancer patients (13). The semi-quantitative ER, PR, Ki-67 and HER2 results of IHC analysis were used to calculate a risk score, known as the IHC4 score, using weighting factors and an algorithm. The score was found to provide prognostic information independent of traditional histopathologic variables and demonstrated prognostic utility similar to the 21-gene recurrence score (RS) assay. In a subsequent study , the IHC4+C score (which also incorporates clinicopathologic parameters) reclassified more than half of patients stratified as intermediate-risk into the low-risk category.
Another option for multiple-biomarker evaluation is the Magee equations. Using several key pathologic parameters like tumor grade, tumor size, and status of ER, PR, HER2 and Ki-67, Klein et al. developed three equations that produced estimated recurrence scores (ERS) highly concordant with the RS assay and useful in breast cancer (14).
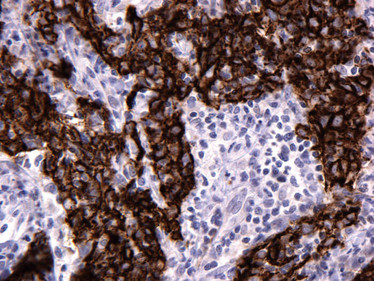
Breast ductal carcinoma (FFPE) stained with anti-E-cadherin.
Is it really that easy?
Despite its helpfulness and the variety of available markers, IHC analysis for breast cancer is not entirely cut-and-dried. There’s still some concern about the lack of reliability and reproducibility of IHC analysis in routine clinical settings as a result of poor assay standardization. A wide range of factors can impact the quality of tissue samples for IHC analysis, including tissue handling, fixation, antibody reagents, staining protocols and the pathologists’ interpretation of the assay results. The American Society of Clinical Oncology and the College of American Pathologists published guidelines for HER2 and ER/PR testing (18), (19) in an effort to improve test quality, inter-laboratory agreement and test reliability for breast cancer patients – so those guidelines now serve as a reference for laboratories undertaking molecular tests. There’s also a need for caution when performing IHC analysis on decalcified or alcohol-fixed specimens, because most such tests aren’t validated in those types of specimens.
Traditionally, IHC analysis has been used only to aid in diagnosis. But with the development of targeted therapies for ER and HER2, testing for expression of these biomarkers has become an assay with treatment implications – and the possibilities for new personalized treatments are increasing every day, so it’s not unreasonable to expect other tests to go the same way. The use of combination IHC biomarkers as surrogates for molecular classification and other multi-gene prognostic panels has also intensified the focus on immunohistochemical analysis, and means that – if the proper precautions are taken for quality control and independent verification – IHC can continue to become an ever more prominent tool in the quest to defeat
breast cancer.
Ping Tang is a Professor and the Director for breast pathology in the Department of Pathology and Laboratory Medicine at the University of Rochester, USA.
- P Tang et al., White Paper, Agilent Technologies (2016).
- R Dewar et al., Arch Pathol Lab Med; 135, 422–429 (2011). PMID: 21466356.
- CB Hill, IT Yeh, Am J Clin Pathol, 12336-1244 (2005). PMID: 1576227.
- Y Otsuki et al., Pathol Int, 57, 421–429 (2007). PMID: 17587241.
- WD Dupont, DL Page, N Engl J Med, 312, 146–151 (1985). PMID: 3965932.
- PM Fitzgibbons et al., Arch Pathol Lab Med, 122, 1053–1055 (1998). PMID: 9870852.
- N Sneige et al., Mod Pathol;15, 1044–1050 (2002). PMID: 12379750.
- SJ Shin et al., Hum Pathol, 44, 1998–2009 (2013). PMID: 23809857.
- DJ Dabbs et al., Am J Surg Pathol, 31, 427–437 (2007). PMID: 17325485.
- MM Koker, CG Kleer, Am J Surg Pathol, 28, 1506–1512 (2004). PMID: 15489655.
- EV Jensen, VC Jordan, Clin Cancer Res, 9, 1980–1989 (2003). PMID: 12796359.
- G Arpino et al., J Natl Cancer Inst, 97, 1254–1261 (2005). PMID: 16145046.
- J Cuzick et al., J Clin Oncol, 29, 4273–4278 (2011). PMID: 21990413.
- M Klein et al., Modern Pathol, 26, 658–664 (2013).
- S Loi et al., Ann Oncol, 25, 1544–1550 (2014). PMID: 24608200.
- SP Patel, R Kurzrock, Mol Cancer Ther, 14, 847–856 (2015). PMID: 25695955.
- P Tang, G Tse, Arch Pathol Lab Med, [In press] (2016).
- ME Hammond et al., Arch Pathol Lab Med, 134, e48–e72 (2010). PMID: 20586616.
- AC Wolff et al., Arch Pathol Lab Med, 138, 241–256 (2014). PMID: 24099077.
Ping Tang is a Professor and the Director for breast pathology in the Department of Pathology and Laboratory Medicine at the University of Rochester, USA.